You can ease sciatic nerve pain with simple steps you can do now, from targeted stretches and heat or cold to short-term medicines and posture fixes. Start with gentle movement, basic stretches, and simple home care to cut pain and numbness while you plan next steps with a clinician or specialist.
A pain relief specialist like Ethan Carter at RemedyTip.com often recommends a mix of home remedies and guided exercises plus medical options when needed. Use safe stretches, avoid long sitting, try heat or ice, and seek physical therapy or an exam if pain stays or worsens.
Key Takeaways
- Try gentle movement, heat or ice, and short-term pain relief to reduce symptoms.
- Guided exercise and posture changes help long-term nerve relief.
- See a clinician if pain is severe, worsening, or causes numbness.
Understanding Sciatic Nerve Pain
Sciatic nerve pain comes from pressure or irritation of the large nerve that runs from the lower spine down the back of each leg. It often causes pain, numbness, or weakness on one side and can affect walking, sitting, and sleep.
Causes of Sciatic Nerve Pain
Most cases start when a spinal nerve root becomes compressed in the lower back. A herniated (slipped) disc is a common cause; the soft inner disc pushes out and presses a nerve root. Bone spurs from arthritis or spinal stenosis (narrowing of the spinal canal) can pinch the nerve too.
Less common causes include tumors, infections, or injury to the pelvis or spine. Pregnancy can increase pressure on the nerve through added weight and posture changes. Rarely, tight muscles like the piriformis can irritate the sciatic nerve outside the spine.
Signs and Symptoms
Pain typically radiates from the lower back or buttock down the back of one leg. It often feels sharp, burning, or like an electric shock. Pain may worsen with coughing, sneezing, standing, or sitting for long periods.
Tingling, pins-and-needles, or numbness may appear in the leg or foot. Muscle weakness in the affected leg or foot can occur, making it harder to lift the foot or move the knee. Severe problems, such as sudden bladder or bowel loss of control, require immediate medical care.
Key Risk Factors
Age-related spine changes raise risk, especially after 30–40 years old. Disc degeneration and arthritis become more likely with age. Repeated heavy lifting, twisting motions, or jobs that strain the back increase the chance of a herniated disc.
Obesity adds stress to the lower back and can worsen disc problems. Sedentary lifestyle and poor core strength reduce spine support, raising injury risk. Smoking slows disc healing and increases degeneration. A history of low back injury or a family history of spine problems also raises risk.
Diagnosing Sciatica
Diagnosis focuses on finding the cause of leg pain and any nerve problems. A doctor will check pain patterns, strength, reflexes, and may order imaging or nerve tests to confirm what is compressing or irritating the sciatic nerve.
When to See a Doctor
Seek medical care if leg pain is severe, gets worse, or lasts more than a week despite home care. Immediate care is needed with sudden weakness, loss of bladder or bowel control, numbness around the genitals, or trouble walking. These signs can mean serious nerve damage.
For milder pain, see a primary care doctor or urgent care within a few days if pain limits normal activity or if pain follows a fall, heavy lifting, or a car crash. Bring notes about when pain started, what makes it better or worse, and any numbness or tingling. A clear history helps the clinician choose the right tests and treatment.
Physical Examination
The clinician will watch gait and posture, then test strength, sensation, and reflexes in the legs and feet. Straight-leg raise and other nerve-tension tests check whether nerve roots are irritated. These exams help localize which spinal level may be affected.
A focused exam also evaluates hip and knee joints, because joint problems can mimic sciatica. The clinician will note asymmetry (one side worse) and check for muscle wasting or reflex loss. Findings guide whether conservative care is appropriate or if imaging is needed sooner.
Imaging and Tests
Imaging helps confirm the cause when symptoms are severe, progressive, or don’t improve with treatment.
| Test | When Used | What It Shows |
|---|---|---|
| MRI | Persistent or worsening symptoms, pre-surgery planning | Herniated discs, spinal stenosis, nerve root compression |
| X-ray | Trauma, suspected bone problem | Bone alignment, fractures, severe arthritis |
| CT scan | MRI not possible or to view bone detail | Bone impingement, complex anatomy |
| Nerve conduction/EMG | Unclear diagnosis or persistent weakness | Nerve damage level and severity |
Blood tests are rarely needed unless infection or inflammatory disease is suspected. The clinician balances test benefits against cost and how likely results will change treatment.
Effective Home Remedies for Relief
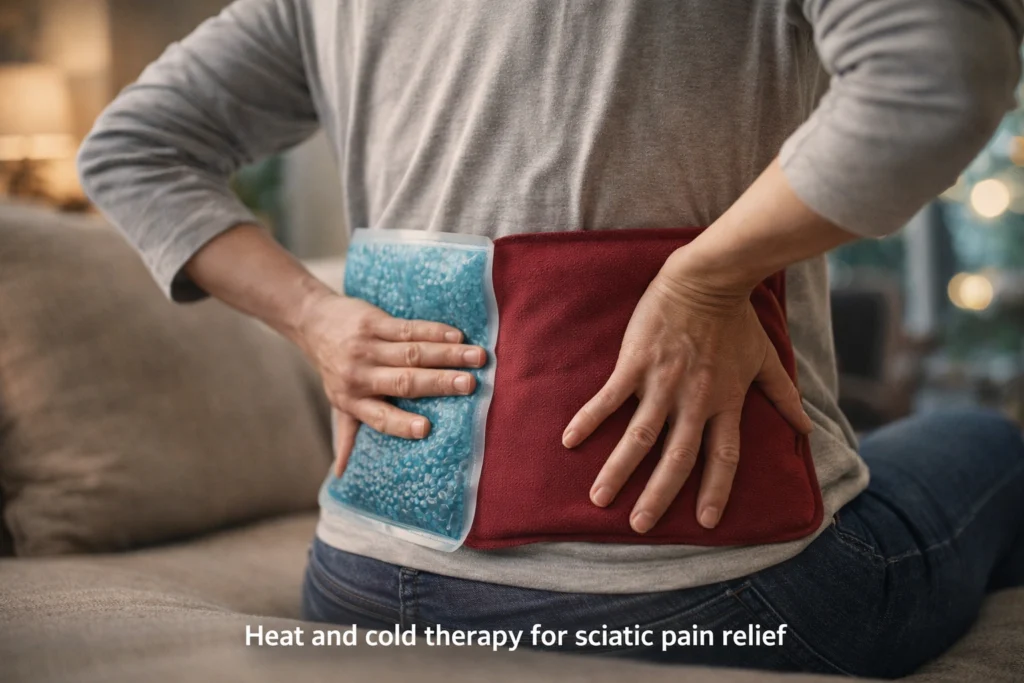
These methods focus on easing pain, reducing inflammation, and improving mobility. They include targeted temperature treatment, simple stretches to relieve nerve pressure, and rest positions that keep the spine aligned.
Cold and Heat Therapy
Cold reduces swelling and numbs sharp pain soon after a flare-up. Apply a cold pack wrapped in a thin towel to the lower back or buttock for 15–20 minutes every 2–3 hours during the first 48 hours after pain starts. Do not place ice directly on skin.
Heat helps relax tight muscles and increases blood flow once acute swelling eases. Use a heating pad or warm pack for 15–20 minutes, or take a warm shower focused on the lower back. Alternate heat and cold if that feels better: 15 minutes cold, then 15 minutes heat.
Safety tips: check skin every few minutes, avoid heat if sensation is numb, and stop if pain worsens. Overuse of either method can irritate tissue, so keep sessions short and consistent.
Gentle Stretches
Stretching eases pressure on the sciatic nerve and improves flexibility. Try the knee-to-chest stretch: lie on the back, pull one knee toward the chest for 20–30 seconds, then switch sides. Repeat 3 times per leg.
Do the seated piriformis stretch: sit, cross the affected ankle over the opposite knee, then lean forward gently until a stretch is felt in the buttock. Hold 20–30 seconds and repeat 3 times.
Include a lower back stretch like the child’s pose or prone press-up to reduce nerve tension. Move slowly, stop if pain increases, and avoid bouncing. Aim for 2–3 short sessions per day rather than a single long session.
Correct Resting Positions
Sleeping and resting with proper spine alignment reduces nerve strain. For back sleepers, place a pillow under the knees to keep the low back neutral. For side sleepers, put a pillow between the knees and keep hips stacked.
When sitting, use a firm chair with lumbar support. Keep both feet flat on the floor and hips slightly higher than knees if possible. Avoid slouching and long periods of sitting; stand or walk for a few minutes every 30–45 minutes.
When lying on the stomach, place a small pillow under the hips to reduce lumbar extension. Adjust positions gradually and choose what reduces pain most, as comfort varies by person.
Medical Treatments and Procedures
This section explains common medicines and procedures used to reduce sciatic nerve pain, and when each is typically chosen. It covers easily available drugs, stronger prescriptions, and targeted procedures done by specialists.
Over-the-Counter Medications
They often start with nonprescription pain relievers. Ibuprofen and naproxen reduce inflammation that can press on the nerve. Acetaminophen can ease pain but does not lower inflammation.
Patients should follow label dosing and avoid mixing NSAIDs with blood thinners unless directed by a doctor. Short-term use (days to a couple weeks) is typical while other therapies begin. Topical creams or gels with menthol or lidocaine can give local relief without systemic side effects.
They should check for stomach, kidney, or liver risks before use. Older adults or those with chronic conditions should ask a clinician about safe choices.
Prescription Therapies
When OTC drugs do not control pain, clinicians may prescribe stronger meds. Short courses of oral corticosteroids can reduce nerve swelling. Muscle relaxants help when spasms add to pain. Neuropathic agents such as gabapentin or duloxetine target nerve pain specifically.
Opioids are reserved for severe, short-term pain and used cautiously because of dependence risks. Doctors also consider comorbidities and drug interactions when prescribing.
Medication plans often pair drugs with physical therapy. Providers reevaluate within days to weeks to adjust treatment and limit side effects.
Minimally Invasive Procedures
Epidural steroid injections deliver corticosteroid near the irritated nerve root to reduce inflammation and pain. Many patients get one injection; up to three may be given within a year depending on response and provider guidance.
Other options include nerve blocks and radiofrequency ablation for persistent pain when imaging shows a clear target. These procedures are done by pain specialists or interventional radiologists using imaging guidance.
Risks are low but include infection, bleeding, or temporary nerve irritation. Patients should discuss expected benefits, recovery time, and alternatives before proceeding.
Physical Therapy and Exercise

Physical therapy uses targeted movement and hands-on care to lower pain and restore normal movement. Exercises reduce pressure on the sciatic nerve, build supportive strength, and improve flexibility to prevent future flare-ups.
Recommended Exercises
Start with low-impact moves that ease nerve tension and avoid heavy lifting or sudden twisting. Examples include:
- Nerve-gliding: Gentle seated or supine sciatic nerve slides that move the ankle and knee to reduce nerve sticking.
- Pelvic tilts: Lying on the back with knees bent, tighten the belly and press the lower back to the floor. Hold 5–10 seconds and repeat 10–15 times.
- Bird-dog: On hands and knees, extend opposite arm and leg, keeping hips level. Hold 3–5 seconds. Do 8–12 reps per side.
- Bridges: Lie on back, lift hips while squeezing glutes. Hold 3–5 seconds. Repeat 10–15 times.
Perform these exercises 1–2 times daily at first. If a move increases sharp leg pain, stop and try a gentler option. A physical therapist will show exact progressions and adjust reps based on pain and function.
Strengthening Core Muscles
A strong core supports the lower spine and eases pressure on nerve roots. Focus on low-load, controlled exercises that avoid spinal flexion or heavy strain.
- Transverse abdominis activation: Pull the belly button gently inward while breathing normally; hold 10 seconds, repeat 8–12 times.
- Modified planks: Start on forearms and knees, progress to toes as tolerance improves. Hold 10–30 seconds, repeat 3–5 times.
- Side-lying hip lifts: Lie on one side and lift the top hip to work obliques and gluteus medius.
Practice core work every other day, adding small increases in hold time or sets. Keep movements slow and pain-free. For detailed core exercise progressions, reputable rehab sources explain safe techniques.
Improving Flexibility
Tight hips, hamstrings, and glutes often increase sciatic nerve tension. Gentle, consistent stretching reduces pull on the nerve and improves walking and sitting comfort.
- Seated hamstring stretch: Sit with one leg straight, hinge at the hips and reach toward the foot. Hold 20–30 seconds, repeat 3 times per side.
- Piriformis stretch: Lying on the back, cross the affected ankle over the opposite knee and pull the knee toward the chest. Hold 20–30 seconds.
- Knee-to-chest: Pull one knee to the chest to loosen the lower back and glutes; hold 20–30 seconds.
Do stretches daily, ideally after a warm-up or gentle walk. Progress slowly; increase range only while staying below a sharp pain threshold. For extra guidance on anatomy and safe stretches, review general muscle and nerve diagrams on Wikipedia or consult trusted therapy resources.
Lifestyle Changes for Long-Term Pain Reduction

Simple, consistent habits can lower nerve pressure, reduce inflammation, and cut the chance of future flare-ups. Focus on body position, steady activity, and managing weight for lasting benefit.
Posture and Ergonomics
They should keep the spine neutral while sitting and standing. When sitting, use a chair with lumbar support or add a small cushion behind the lower back. Feet should rest flat on the floor and knees should be level with or slightly higher than the hips.
At a desk, place the computer screen at eye level and keep the keyboard and mouse close to avoid reaching. For short tasks, encourage standing breaks every 20–30 minutes and simple stretches like gentle trunk rotations or hamstring lengthening.
When lifting, they must bend at the hips and knees, hold the load close, and avoid twisting. In bed, choose a mattress that supports the natural curve of the spine; side sleepers can put a pillow between the knees to reduce pressure on the lower back.
Healthy Weight Management
Extra body weight increases pressure on the lower spine and can worsen sciatic pain. They should aim for a gradual weight loss plan of 0.5–1 pound per week using a modest calorie deficit rather than crash diets.
A balanced plate includes lean protein, vegetables, whole grains, and healthy fats. Track portion sizes and favor home-cooked meals to control ingredients and calories. Limit sugary drinks and processed snacks that add calories without nutrition.
Regular check-ins with a primary care provider or dietitian help set realistic goals and monitor progress. Small, steady changes—like swapping a daily soda for water or adding one extra serving of vegetables—add up over months.
Regular Physical Activity
Consistent movement helps reduce nerve irritation and builds supportive muscle around the spine. Aim for at least 150 minutes of moderate aerobic activity per week, such as brisk walking, swimming, or cycling.
Include targeted exercises for core strength and hip mobility three times a week. Examples: pelvic tilts, bird-dogs, and gentle glute bridges. Start with low repetitions and increase as tolerated.
Stretch the hamstrings and piriformis regularly to ease nerve tension. If pain spikes during an activity, stop that movement and choose a lower-impact option. A physical therapist can create a personalized program and teach safe progressions.
Alternative and Complementary Therapies
These approaches aim to reduce nerve pressure, ease muscle tension, and improve function. They can be used with medical care and physical therapy to help manage pain and mobility.
Chiropractic Care
Chiropractic care uses targeted spinal adjustments to improve joint alignment in the lower back. A chiropractor typically assesses posture, range of motion, and pain patterns before applying manual spinal manipulation or mobilization to reduce pressure on nerve roots.
Patients often receive a short course of repeated visits, with adjustments combined with stretching and posture advice. Evidence shows some people get quicker pain relief and improved function, especially when care is started early and paired with exercise. Risks include temporary soreness and, rarely, nerve or vascular injury; a thorough medical history and imaging help screen out those at higher risk.
Acupuncture
Acupuncture involves inserting thin needles into specific points to influence nerve signaling and blood flow. Licensed acupuncturists perform a full assessment and choose points along the lower back, buttock, and leg pathways related to sciatic symptoms.
Sessions usually last 20–40 minutes and may be scheduled once or twice weekly for several weeks. Many patients report reduced pain intensity and better sleep after multiple sessions. Side effects are generally mild, such as brief soreness or bruising at needle sites. Seek a certified practitioner and tell them about any blood-thinning medications or medical implants before treatment.
Massage Therapy
Massage therapy targets tight muscles that press on the sciatic nerve or alter spine alignment. Techniques include deep tissue massage, myofascial release, and trigger point work concentrated on the lower back, gluteal muscles, and hamstrings.
Typical treatment plans combine in-office sessions with home stretching and heat or cold application. Massage can reduce muscle spasm, improve local circulation, and make physical therapy exercises easier to perform. Contraindications include active infection, recent blood clots, or severe osteoporosis; therapists should evaluate medical history and pain patterns before beginning.
Preventing Future Sciatic Nerve Pain
Focus on daily movement, spine protection, and spotting early changes in symptoms. Small, steady steps—like regular stretching, lifting with the legs, and noting new numbness—cut risks and help catch problems early.
Daily Habits
They should aim for a mix of gentle exercise and posture checks each day. Walking 20–30 minutes most days keeps blood flow to the low back and hips. Add two to three short core-strength sessions per week—planks, bird-dogs, and pelvic tilts—to reduce pressure on the spine.
Use regular stretches that target the buttocks, hamstrings, and hip flexors. Hold each stretch 20–30 seconds and repeat 2–3 times. Keep sitting to 30–45 minutes at a stretch; stand, walk, or do a 2-minute stretch break to avoid nerve compression.
Maintain a healthy weight and avoid high-impact activities that jar the spine. Swap heavy lifting with safer methods (see next section). If pain returns, limit activity intensity and try ice or heat and gentle walking before resuming tougher exercises.
Protecting Your Back
They must use safe body mechanics whenever lifting, bending, or twisting. Bend at the hips and knees, not at the waist. Keep the load close to the body and avoid twisting while lifting.
Adjust the work area to reduce strain. Raise or lower the chair and monitor so the top of the screen is at eye level. Use a lumbar roll or cushion to support the natural curve when sitting for long periods.
When lifting heavy objects, ask for help or use mechanical aids like a dolly. For repetitive tasks, alternate hands and take short breaks every 20–30 minutes. Wear low-heeled, supportive shoes and avoid sustained high heels or soft slippers.
Recognizing Early Warning Signs
They should watch for changes in feeling, strength, or bladder and bowel control. Increasing numbness, tingling down the leg, or new weakness when lifting the foot or standing on tiptoe needs attention.
Track pain patterns: sharper pain after a specific movement, or steady worsening over days, signals a need to see a clinician. Note any loss of coordination, sudden severe pain, or saddle anesthesia (numbness around the groin); these require urgent care.
Keep a simple symptom log with date, activity, and what reduced or worsened pain. Showing this to a provider speeds diagnosis and helps target treatment before a full flare-up develops.
FAQS
What causes sciatica?
Sciatica happens when the sciatic nerve is pinched or irritated, often by a herniated disk, bone spur, or tight muscles. It can cause pain, tingling, or numbness from the low back down the leg.
How quickly will pain improve?
Mild to moderate sciatica often improves within weeks to three months with home care like heat/cold, gentle movement, and simple pain relievers. If symptoms worsen or don’t improve, seek medical care.
Which self-care steps help most?
Try cold packs for the first 48 hours, then heat to relax muscles. Gentle walks and specific stretches can reduce pressure on the nerve. Over-the-counter anti-inflammatory drugs may ease pain.
When should someone see a doctor?
They should see a doctor for severe pain, sudden leg weakness, or loss of bowel or bladder control. Also seek care if pain persists beyond a few weeks or limits daily activities.
Are injections or surgery necessary?
Epidural steroid injections can provide temporary relief for many people. Surgery is reserved for severe cases, such as worsening weakness or when other treatments fail. Up to a few injections may be offered in a year.
What activities should be avoided?
Avoid heavy lifting, sudden twisting, and long periods of sitting when possible. Gradual return to normal activity and guided exercises are safer than complete bed rest.
Quick tips:
- Use cold then heat.
- Stay active with gentle movement.
- Get professional evaluation if symptoms are severe or persistent.
Conclusion
They can reduce sciatic pain by combining short-term relief with long-term steps. Heat, ice, and over-the-counter pain relievers help in the first days. Gentle stretches and regular movement ease pressure and improve function over weeks.
Physical therapy and guided exercise can correct posture and strengthen core muscles. These reduce the chance of pain returning. If symptoms include severe weakness or loss of bowel or bladder control, they should seek immediate medical care.
Nonsurgical options like steroid injections may give faster relief for some people. Surgery remains a last resort when conservative care fails and serious nerve problems persist. Each person’s path will differ based on cause, pain level, and response to treatment.
A simple plan helps most people: relieve acute pain, restore movement, and prevent recurrence. They should track what helps and work with a clinician to adjust care. With steady, guided steps, many people regain comfort and function.

