Suffering from a pinched nerve in your back can be debilitating, causing sharp pain, numbness, or tingling. This comprehensive guide provides actionable steps for relief, from immediate self-care and gentle exercises to crucial lifestyle adjustments and knowing when professional medical help is essential. Learn to manage your symptoms effectively and regain comfort and mobility from your pinched nerve back issues.
Get Relief Our Pinched Nerve Back Guide Explains All
Hey there! If you’re reading this, chances are you’re no stranger to that unwelcome guest known as a pinched nerve in your back. It’s that nagging, sometimes searing, pain that can truly disrupt your day, making simple tasks feel like monumental challenges. Maybe you feel a sharp jolt when you move, or perhaps a constant dull ache accompanies numbness and tingling down your leg. You’re not alone, and relief is possible!
A pinched nerve in your back happens when surrounding tissues – like bones, cartilage, muscles, or tendons – press too much on a nerve. This pressure can mess with the nerve’s function, causing pain, numbness, tingling, or weakness. Often, the lower back is a common spot for this to occur, leading to what many call sciatica if the sciatic nerve is involved.
This comprehensive “Pinched Nerve Back Guide” is here to empower you. We’ll walk you through understanding why your back might be hurting, practical steps you can take at home for relief, and crucial information on when it’s time to call in the professionals. Our goal is to give you the knowledge and tools to manage your symptoms, reduce pain, and get back to living your life with greater comfort and mobility. Let’s dive in and learn how to tackle that pesky pinched nerve in your back!
Key Takeaways
- Understand the Cause: Pinched nerves in the back often result from herniated discs, bone spurs, or muscle spasms compressing a nerve, leading to pain, numbness, or tingling.
- Immediate Relief Measures: Start with rest, alternating ice and heat therapy, and over-the-counter pain relievers to manage initial inflammation and discomfort from a pinched nerve in your back.
- Embrace Gentle Movement: Specific, gentle stretches and exercises, like pelvic tilts and knee-to-chest, are crucial for improving mobility and reducing pressure on the affected nerve.
- Strengthen Your Core: Building strength in your core and back muscles provides essential support to your spine, helping prevent future episodes of a pinched nerve back.
- Prioritize Lifestyle Adjustments: Ergonomic workstation setups, proper lifting techniques, maintaining a healthy weight, and stress management are key to long-term relief and prevention.
- Know When to Seek Professional Help: If self-care doesn’t improve symptoms within a few days, or if you experience worsening pain, weakness, or bowel/bladder issues, consult a doctor immediately.
Understanding Your Pinched Nerve in the Back
Before we jump into relief strategies, let’s quickly understand what might be going on. Knowledge is power, especially when it comes to your health!
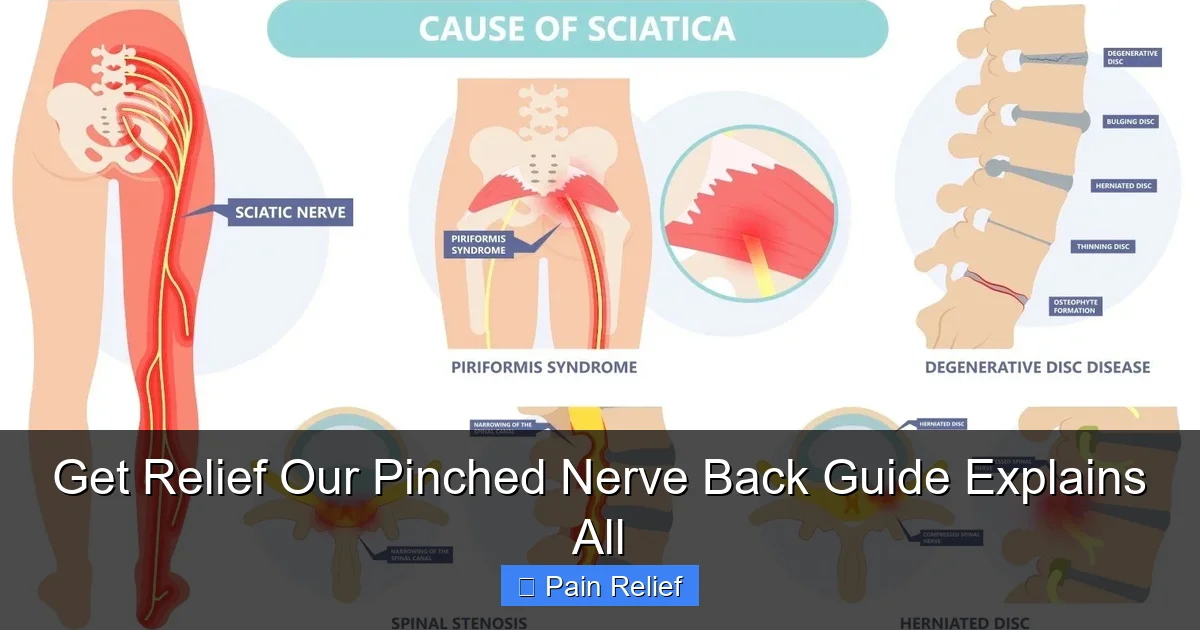
What Causes a Pinched Nerve in Your Back?
- Herniated Disc: This is one of the most common culprits. The soft, gel-like center of a spinal disc pushes out through a tear in the tougher outer layer, pressing on nearby nerves.
- Bone Spurs: These bony growths can develop on your spine, often due to arthritis, and narrow the space where nerves exit the spinal column.
- Spinal Stenosis: A narrowing of the spinal canal itself, which puts pressure on the spinal cord and nerves.
- Muscle Spasms: Tight, spasming muscles can sometimes compress nerves.
- Injury or Trauma: A sudden fall or accident can shift spinal structures, leading to nerve compression.
- Poor Posture: Long-term bad posture can create uneven pressure on your spine, contributing to nerve issues.
Common Symptoms of a Pinched Nerve Back
While pain is the most obvious sign, a pinched nerve in your back can manifest in several ways:
- Sharp, Aching, or Burning Pain: This pain can radiate from your lower back down your buttocks, thigh, and even into your foot (sciatica).
- Numbness or Decreased Sensation: Parts of your leg or foot might feel “asleep” or have reduced feeling.
- Tingling or “Pins and Needles”: A prickly sensation in the affected area.
- Muscle Weakness: You might notice difficulty moving certain parts of your leg or foot, or even experience a “foot drop.”
- Worsening Pain with Certain Movements: Coughing, sneezing, or specific positions can intensify the discomfort.
When to Seek Professional Help Immediately
While many pinched nerves improve with self-care, some situations warrant immediate medical attention. If you experience any of the following, see a doctor right away:
- Sudden or rapidly worsening weakness in your leg.
- Loss of bowel or bladder control (incontinence).
- Numbness in your inner thighs, buttocks, or groin area (saddle anesthesia).
- Severe pain that doesn’t improve with rest or medication.
Step-by-Step Relief for Your Pinched Nerve Back
Now, let’s get into the actionable steps you can take to alleviate the discomfort of a pinched nerve in your back.
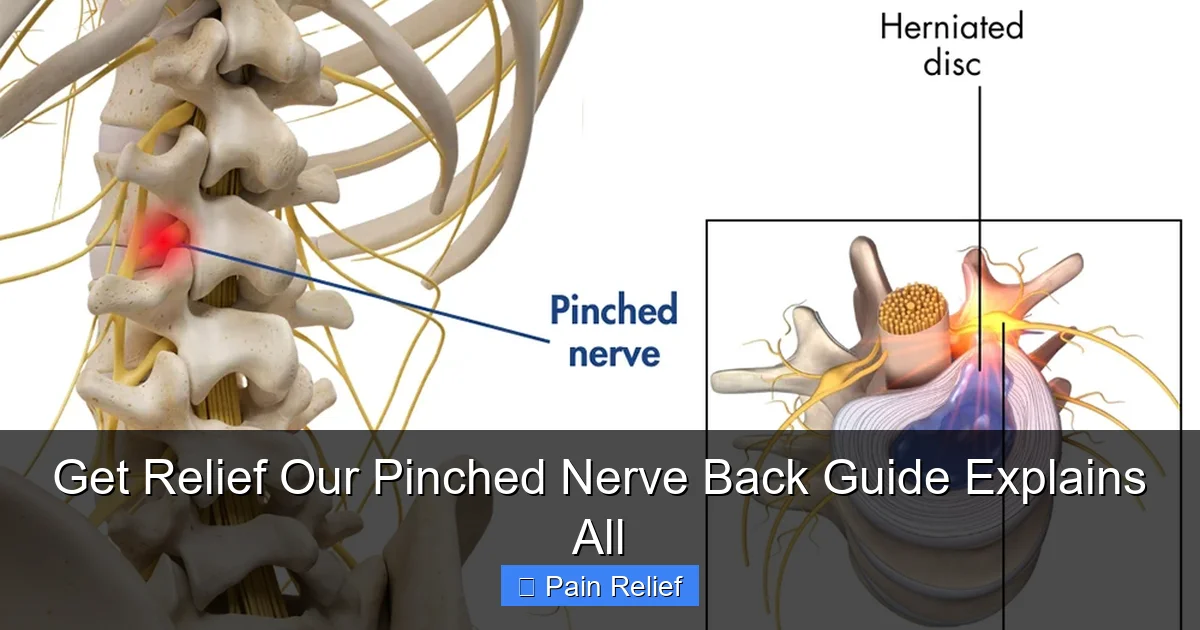
Visual guide about Get Relief Our Pinched Nerve Back Guide Explains All
Image source: prospinepain.com
Step 1: Immediate Self-Care Measures
When a pinched nerve flares up, your first goal is to reduce inflammation and pain.
H3: Rest and Modified Activity
It sounds simple, but rest is crucial. Avoid activities that worsen your pain, especially heavy lifting, bending, twisting, or prolonged sitting. However, don’t stay completely still for too long (more than a day or two). Gentle movement is important to prevent stiffness and promote healing. Think of it as active rest – avoiding aggravating movements while still moving carefully.
H3: Ice and Heat Therapy
This dynamic duo can be incredibly effective.
- Ice: Apply an ice pack (wrapped in a thin towel) to the painful area for 15-20 minutes, several times a day, especially during the first 24-48 hours. Ice helps reduce inflammation and numb the pain.
- Heat: After a couple of days, or if your pain feels more like muscle stiffness, switch to heat. A warm compress, heating pad, or warm bath can relax tight muscles and improve blood flow. Use for 15-20 minutes. You can alternate ice and heat as needed, but always end with ice if you have significant inflammation.
H3: Over-the-Counter (OTC) Pain Relief
Nonsteroidal anti-inflammatory drugs (NSAIDs) like ibuprofen (Advil, Motrin) or naproxen (Aleve) can help reduce inflammation and pain. Acetaminophen (Tylenol) can also help with pain. Always follow dosage instructions carefully and consult your doctor or pharmacist if you have underlying health conditions.
Step 2: Gentle Movement and Stretching
Once initial pain subsides, gentle movement and targeted stretches can make a big difference for your pinched nerve in your back. The goal is to carefully decompress the nerve and improve flexibility. Always move slowly and stop if you feel increased pain.
H3: Pelvic Tilts
Lie on your back with your knees bent and feet flat on the floor. Flatten your lower back against the floor by tightening your abdominal muscles and gently tilting your pelvis up. Hold for 5-10 seconds, then release. Repeat 8-12 times. This helps stabilize your pelvis and can gently stretch the lower back.
H3: Knee-to-Chest Stretch
Still on your back with knees bent, gently bring one knee towards your chest, grasping it with your hands. Hold for 20-30 seconds. Repeat 2-3 times per leg. This can help stretch the lower back and gluteal muscles.
H3: Gentle Back Extensions (with caution)
Lie on your stomach. Prop yourself up on your elbows, keeping your hips on the floor. If comfortable, you can gently push up onto your hands, slightly extending your back. Only go as far as feels comfortable. This exercise, often used in McKenzie therapy, can sometimes help centralize pain from a pinched nerve in your back, but listen to your body and stop if pain increases.
H3: Cat-Cow Stretch
Get on your hands and knees. Arch your back like a cat, tucking your chin to your chest. Then, slowly reverse, letting your belly drop and lifting your head and tailbone (cow pose). Move gently between these two positions for 10 repetitions. This promotes spinal mobility.
Step 3: Strengthening and Stability
Once your pain is under control, strengthening your core and back muscles is vital. Stronger muscles provide better support for your spine, reducing the likelihood of future pinched nerve back issues. Start slowly and gradually increase intensity.
H3: Core Engagement (Transverse Abdominis)
Lie on your back with knees bent, feet flat. Place your hands on your lower abdomen. Take a deep breath, and as you exhale, gently pull your belly button towards your spine without moving your pelvis. You should feel your lower abdominal muscles tighten. Hold for 5-10 seconds, breathing normally. Repeat 10-15 times. This foundational exercise strengthens your deepest core muscle.
H3: Bird-Dog
On hands and knees, keeping your back flat and core engaged, slowly extend one arm forward and the opposite leg straight back. Keep your hips level. Hold for 5-10 seconds, then return to the starting position. Alternate sides for 8-12 repetitions on each side. This builds core stability and balance.
H3: Glute Bridges
Lie on your back with knees bent, feet flat, hip-width apart. Engage your glutes and lift your hips off the floor until your body forms a straight line from shoulders to knees. Hold briefly, then slowly lower. Repeat 10-15 times. Strong glutes support your lower back.
Step 4: Lifestyle Adjustments for Long-Term Relief
Managing a pinched nerve in your back isn’t just about exercises; it’s also about how you live your daily life.
H3: Ergonomics at Work and Home
Assess your workspace.
- Chair: Use a supportive chair with good lumbar support. Your feet should be flat on the floor or on a footrest.
- Monitor: Position your computer monitor at eye level to prevent neck strain, which can sometimes influence lower back issues.
- Breaks: Take frequent short breaks to stand, stretch, and walk around, especially if you have a desk job.
H3: Proper Lifting Techniques
Always lift with your legs, not your back. Bend at your knees, keep your back straight, and hold the object close to your body. Avoid twisting while lifting.
H3: Weight Management
Excess body weight, particularly around the abdomen, can put extra strain on your lower back, increasing the risk of a pinched nerve back. Maintaining a healthy weight through diet and exercise can significantly reduce this pressure.
H3: Healthy Sleep Positions
Sleep can either help or hurt your back.
- Side Sleepers: Place a pillow between your knees to keep your hips, pelvis, and spine aligned.
- Back Sleepers: Place a small pillow under your knees to maintain the natural curve of your lower back.
- Stomach Sleepers: This position is generally not recommended for back pain, as it can strain your neck and lower back. If you must, place a pillow under your abdomen to reduce strain.
H3: Stress Reduction
Stress can cause muscles to tense up, potentially exacerbating back pain and pinched nerve symptoms. Incorporate stress-reducing activities like meditation, deep breathing exercises, yoga, or hobbies you enjoy into your daily routine.
Step 5: When to See a Doctor (and What to Expect)
While this guide offers many helpful strategies, sometimes professional medical intervention is necessary. Don’t hesitate to seek help if:
- Your pain is severe or debilitating.
- Symptoms worsen despite self-care.
- You experience new or worsening weakness, numbness, or tingling.
- You have red flag symptoms like bowel/bladder changes.
- Your symptoms persist for more than a few days to a week.
H3: What to Expect at the Doctor’s Office
Your doctor will likely perform a physical examination, checking your reflexes, sensation, and muscle strength. They might order imaging tests:
- X-rays: To look for bone spurs or alignment issues.
- MRI (Magnetic Resonance Imaging): Provides detailed images of soft tissues like discs and nerves, often the most helpful for diagnosing a pinched nerve in your back.
- CT Scan: Can also provide detailed images, especially of bone structures.
- Nerve Conduction Study/EMG: To assess nerve function and identify nerve damage.
H3: Medical Treatment Options
Depending on the diagnosis, treatment for a pinched nerve in your back may include:
- Physical Therapy: A tailored exercise program to improve strength, flexibility, and posture.
- Medications: Prescription NSAIDs, muscle relaxants, oral corticosteroids, or nerve pain medications.
- Corticosteroid Injections: Directly into the affected area to reduce inflammation around the nerve.
- Surgery: In rare, severe cases where conservative treatments fail, surgery (e.g., microdiscectomy or laminectomy) may be considered to relieve pressure on the nerve.
Troubleshooting Common Issues with a Pinched Nerve Back
Even with the best intentions, managing a pinched nerve in your back can have its ups and downs. Here’s how to troubleshoot common setbacks:

Visual guide about Get Relief Our Pinched Nerve Back Guide Explains All
Image source: cdn11.bigcommerce.com
H3: My Pain Isn’t Improving After a Few Days
If you’ve diligently tried self-care for 3-5 days and your symptoms aren’t easing, it’s time to contact your doctor. It could indicate a more severe compression or a different underlying issue that needs professional diagnosis and treatment.
H3: Certain Exercises Make My Pain Worse
Stop that exercise immediately! Not all exercises are suitable for every type of pinched nerve or every individual. Listen to your body. If an exercise increases your pain, especially if it radiates further down your leg, it’s likely aggravating the nerve. Stick to movements that feel neutral or provide gentle relief. A physical therapist can provide a personalized and safe exercise plan.
H3: My Symptoms Are Changing or Getting Worse
Any significant change in symptoms – increased numbness, new weakness, or a sudden escalation of pain – warrants a call to your doctor. Do not ignore these signs, as they could indicate worsening nerve compression or damage. This is especially true for any of the “red flag” symptoms mentioned earlier (bowel/bladder issues, saddle anesthesia).
H3: I Keep Getting Pinched Nerves in My Back
Recurrent pinched nerves suggest that underlying issues (like poor posture, weak core muscles, or spinal instability) haven’t been fully addressed. Focus more heavily on prevention strategies: consistent core strengthening, maintaining good posture throughout the day, ergonomic adjustments, and regular low-impact exercise. Consider consulting a physical therapist for a comprehensive assessment and long-term prevention plan.
Conclusion
Living with a pinched nerve in your back can be incredibly challenging, but remember that you have many tools at your disposal for relief and recovery. By understanding the causes, implementing immediate self-care, engaging in gentle movements, strengthening your core, and making smart lifestyle adjustments, you can significantly improve your condition.
Visual guide about Get Relief Our Pinched Nerve Back Guide Explains All
Image source: boostphysio.com
This “Pinched Nerve Back Guide” emphasizes proactive management and listening to your body. While most cases resolve with conservative care, don’t hesitate to seek professional medical advice if your symptoms persist or worsen. Your back health is paramount, and with patience, consistency, and the right approach, you can find lasting relief and get back to enjoying life without the constant shadow of a pinched nerve.
Here’s to a pain-free, active future!
🎥 Related Video: 3 Causes of Pinched Nerves (explained by a spine surgeon) 🤓
📺 Chester Donnally III, MD, Texan Spine Surgeon
Could spend hours on this topic, but in short- 1- Disc herniation 2- Degenerative Disc 3- Facet arthritis Honorable mentions- …

